|
For every life saved from breast cancer by the
Breast Cancer Screening Programme, five women are
over-diagnosed, and have to go through an operation
to remove a tumour that otherwise never would have
caused problems. This is one of several conclusions
to an evaluation done by several Scandinavian
researchers.
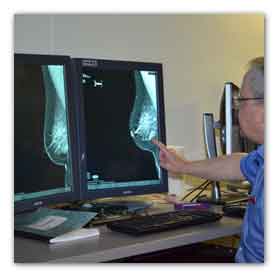
Breast cancer screenings may not lead to fewer
deaths but may lead to overdiagnosis, U.S.
researchers suggest.
In areas of the U.S. with high levels of screening,
more tumors were diagnosed - but breast cancer death
rates were no lower than in areas with fewer
screenings, researchers report.
While screening guidelines vary, the
government-backed U.S. Preventive Services Task
Force says average-risk women should have mammograms
every other year between ages 50 and 74. Getting
screened before age 50 should be an individual
decision, according to the Task Force.
"The mortality results that we observed are far from
definitive," cautioned Charles Harding, the study's
lead author from Seattle, Washington.
Dr. Joann Elmore and Ruth Etzioni of the University
of Washington in Seattle agree in an editorial that
the study's results are limited by the potential of
ecological bias. "Prior ecological studies of
mammography conducted at the larger state level with
a wider range of mammography frequencies showed a
decline in breast cancer mortality associated with
more screening," Elmore and Etzioni added.
The Norwegian government spends NOK 574 million per
screening round to check women between the age of 50
and 69 for breast cancer. An ongoing debate between
Norwegian and international researchers and doctors
considers the wisdom of offering periodic breast
cancer screenings.
On task from the Ministry of Health and Care
Services, the Research Council of Norway has done a
research-based evaluation of the country’s Breast
Cancer Screening Programme.
The evaluation was led by Professor Roar Johnsen at
NTNU (Norwegian University of Science and
Technology).
Together with postdoctoral fellow Signe Opdahl and
the rest of the steering committee, they have gone
through all studies done on mammograms in Norway
since 2008.
The conclusions of these studies, however, are
inconsistent. One report shows that mammograms have
reduced the amount of cancer deaths by 10 per cent,
while another claims as much as 36 per cent. The
evaluation that is now being presented is based on
all of these different studies.
Here are a few of the conclusions in the evaluation:
– Breast cancer deaths have been reduced in Norway
by roughly 20 to 30 per cent as a result of the
screening programme.
– The screening results in overdiagnosis of 15-20
per cent.
– For every 27 women who avoid dying of breast
cancer, 142 women are overdiagnosed and treated
unnecessarily.
– There are a lot of uncertainties in these numbers,
because the studies that the evaluation looked at
are all very different, and because factors such as
the use of mammograms at private clinics and hormone
treatment during menopause are things that most
studies have not been able to consider.
– From a social perspective, the balance between
cost and effect is within the level that health
authorities consider to be acceptable for health
care services.
“The goal of the Breast Cancer Screening Programme
was to reduce breast cancer mortality rates by 30
per cent. Depending on how you look at it, our
estimates show that this goal may have been reached.
But it has taken a huge toll in the form of
overdiagnosis,” says Johnsen.
In 2013, Swiss authorities were advised to end their
breast cancer screening programme, while England was
advised to continue theirs in 2012. Most Western
countries have some kind of screening programme
available.
“One challenge we face is that if a small tumour
that is most likely benign is discovered, we can’t
take the chance of not treating it. This means that
women have to go through cancer treatment, with all
of the social and personal costs it brings
unnecessarily. More money should be given to
research so that we have more knowledge about which
tumours do and do not need treatment. Each
individual woman needs to consider the pros and cons
from her side when she decides if she wants to
participate in the Breast Cancer Screening Programme,”
says Johnsen.
About three quarters of women between 50 and 69
years of age choose to participate in screening.
The evaluation was given to Minister of Health and
Care Services Bent Høie on 5 June.
“We have now presented the basis for a political
decision,” Johnsen concludes.
For more information
Norwegian University of Science and Technology
http://www.ntnu.edu/
Breast Cancer Screening, Incidence, and Mortality
Across US Counties
link...
Effect of Screening Mammography on Cancer Incidence
and Mortality FREE ONLINE FIRST
link...
MDN |