|
Calcium in the arteries of the breast predicts early
buildup of plaque in the heart's arteries, and may
improve risk assessment in many women, especially
young women. Routine mammography may also be a
useful tool to identify women at risk for heart
disease, potentially allowing for earlier
intervention, according to a study scheduled for
presentation at the American College of Cardiology's
65th Annual Scientific Session.
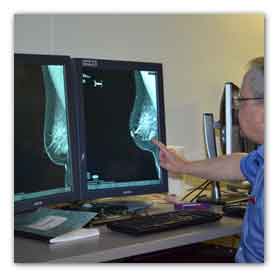
Data from this study show for the first time a link
between the amount of calcium in the arteries of the
breast--readily visible on digital mammography--and
the level of calcium buildup in the coronary
arteries.
Coronary arterial calcification, or CAC, is
considered a very early sign of cardiovascular
disease. Importantly, the presence of breast
arterial calcification also appears to be an
equivalent or stronger risk factor for CAC than
other well-established cardiovascular risk factors
such as high cholesterol, high blood pressure and
diabetes.
Earlier research had shown a link between breast
arterial calcification and atherosclerotic
disease--even heart attack, stroke and other
cardiovascular disease events, but researchers said
these data provide a more direct relationship
between the extent of calcified plaque in the
mammary and coronary arteries, as well as a
comparison to standard risk evaluation.
"Many women, especially young women, don't know the
health of their coronary arteries. Based on our
data, if a mammogram shows breast arterial
calcifications it can be a red flag--an 'aha'
moment--that there is a strong possibility she also
has plaque in her coronary arteries," said Harvey
Hecht, M.D., professor at the Icahn School of
Medicine and director of cardiovascular imaging at
Mount Sinai St. Luke's hospital, and lead author of
the study.
All told, 70 percent of the women who had evidence
of breast arterial calcification on their mammogram
were also found to have CAC as shown on a
noncontrast CT scan of the chest.
For women under 60 years of age with CAC, half also
had breast arterial calcification--an important
finding as very few would be thinking about or
considered for early signs of heart disease.
There were even fewer false positives among younger
patients; researchers said that if a younger woman
had breast arterial calcification, there was an 83
percent chance she also had CAC.
Notably, breast arterial calcification also appeared
to be as strong a predictor for cardiovascular risk
as standard risk scores such as the Framingham Risk
Score, which underestimates women's risk, and the
2013 Cholesterol Guidelines Pooled Cohort Equations,
which tends to overestimate risk, Hecht said. When
researchers added 33 asymptomatic women with
established CAD, breast arterial calcification was
more powerful than both risk assessment formulas,
which suggests the presence of subclinical
atherosclerosis may be a more important indicator of
heart disease than other risk factors.
"This information is available on every mammogram,
with no additional cost or radiation exposure, and
our research suggests breast arterial calcification
is as good as the standard risk factor-based
estimate for predicting risk," Hecht said. "Using
this information would allow at-risk women to be
referred for standard CAC scoring and to be able to
start focusing on prevention--perhaps even taking a
statin when it can make the most difference."
Multivariate analysis showed that early signs of a
buildup of plaque in the coronary arteries were most
strongly related to breast arterial calcification.
While CAC was about two times as likely with
advancing age or high blood pressure, it was three
times more likely with breast arterial
calcification.
"The message is if a woman is getting a mammogram,
look for breast arterial calcification. It's a
freebie and provides critical information that could
be lifesaving for some women," Hecht said, adding he
hopes these findings will prompt clinicians, who
rarely report breast arterial calcification, to
routinely report not just the presence or absence of
breast arterial calcifications but also to estimate
and note the amount.
"The more breast arterial calcification a women has,
the more likely she is to have calcium in her
heart's arteries as well. If all it requires is to
take a closer look at the images, how can we ignore
it?," he said.
A total of 292 women who had digital mammography and
noncontrast CT scans within one year were included
in the study.
Of these, 124, or 42.5 percent, were found to have
evidence of breast arterial calcification.
Mammograms were reviewed by a second radiologist who
was blinded to the CAC results.
Women with breast arterial calcification were more
likely to be older, have high blood pressure and
chronic kidney disease, and less likely smokers.
Women with established cardiovascular diseases were
excluded.
Breast arterial calcification was evaluated on a
scale from zero to 12 by increasing severity, and
CAC was measured on the CT using a validated 0-12
severity score.
The overall accuracy of breast arterial
calcification for the presence of CAC was 70
percent, and 63 percent of those with CAC also had
breast arterial calcification.
To date, there is no consensus on using CAC as a
screening test, though a very large outcome study of
39,000 subjects is underway in the Netherlands.
Mammography, however, is widely used and accepted
and, as Hecht said, may provide an opportunity to
risk stratify asymptomatic women by breast arterial
calcification who might have calcium in the coronary
arteries and ordinarily would not have been readily
considered for cardiovascular screening.
Heart disease is the leading cause of death among
women, yet breast cancer is often the most feared.
Roughly 37 million mammograms are performed annually
in the U.S. Mammography is recommended annually for
women over 40 years of age by the American Cancer
Society and every other year for women 50-75 years
old and women at high risk for breast cancer by the
U.S. Preventive Service Task Force. Digital
mammography is more sensitive to the presence of
calcifications and is now available in 96 percent of
mammography units in the U.S.
Another intriguing point that deserves additional
study, according to the researchers, is that the
nature of the atherosclerosis is different in breast
arterial calcification and CAC, making it unclear
why one should be related to the other.
Hecht stresses that these findings warrant further
evaluation and validation in larger studies. Future
prospective trials are needed to see what the
prognostic significance of breast arterial
calcification might be. Because the study involved
women who received both mammography and CT scan for
clinical indications, these women may have been more
likely than the average woman to have coexisting
conditions, although Hecht said these were unrelated
to heart disease.
In an accompanying editorial in JACC: Cardiovascular
Imaging, Khurram Nasir, M.D., M.P.H., and John
McEvoy, from the Center for Healthcare Advancement
and Outcomes at Baptist Health South Florida, said
that the report provides impetus to document breast
arterial calcification in mammography reports, to
improve education of primary care and radiology
providers on the link with heart disease, and other
actions to establish best practices for
incorporating this research into care.
"Even by the conservative estimate of 10 percent,
approximately 4 million women nationwide undergoing
screening mammography will exhibit breast arterial
calcification; with 2 to 3 million of them likely to
have signs of premature coronary atherosclerotic
disease," the authors said. "Whether the best use of
breast arterial calcification is to trigger
additional testing or to directly inform preventive
treatment decisions, either by flagging high-risk
women to their providers or by reclassifying
traditional (heart disease) risk estimates, is worth
further discussion."
For more information
JACC: Cardiovascular Imaging
Digital Mammography and Screening for Coronary
Artery Disease
Laurie Margolies, MD, Mary Salvatore, MD, Harvey S.
Hecht, MD, Sean Kotkin, MD, Rowena Yip, MPH, Usman
Baber, MD, Vivian Bishay, MD, Jagat Narula, PhD, MD,
David Yankelevitz, MD, Claudia Henschke, PhD, MD.
Link...
MDN |