|
Taking calcium and vitamin D can help prevent broken
bones in older women. However, this benefit may be
cancelled out by an increased risk of heart attack
and stroke.
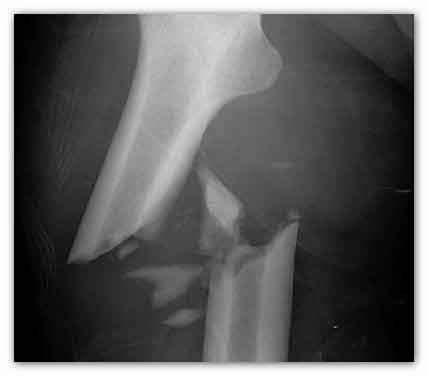
Norway has the highest reported risk of hip
fractures in the whole world. Too little calcium and
vitamin D in your diet leads to an increased risk of
osteoporosis and broken bones, which taking
supplements has been shown to help prevent.
However, some studies have also shown that taking
supplemental calcium may also increase your risk of
heart attack and stroke.
“We conclude that the moderate effect of
supplemental calcium and vitamin D on the risk of
fractures is not large enough to outweigh the
potential increased risk of cardiovascular disease,
specifically in women who are at a low risk of bone
fracture,” said Gunhild Hagen, a PhD candidate at
the Department of Public Heath and General Practice
who was first author of an article on the study
recently published in Osteoporosis International.
Researchers at NTNU and the University of Oslo used
an advanced analytical model to investigate the
total health effect of taking a combined calcium and
vitamin D supplement, compared to taking no
supplements, based on a group of healthy women aged
65 with a BMI of 24 kg/m2.
“Our analysis shows that if 100 000 65-year-old
women take 1000 mg calcium every day, 5890 hip
fractures and 3820 other fractures would be
prevented.
On the other hand, as many as 5917 heart attacks and
4373 strokes could be caused. So for women of this
age, the risks outweigh the benefits,” the authors
of the study wrote in an article in Aftenposten, one
of Norway’s national newspapers.
Recent studies of the effect of calcium
supplementation on the risks of heart attack and
stroke have reached conflicting conclusions, so the
researchers used three different scenarios based on
results from previous studies.
The high-risk model predicted that more than 10 000
heart attacks and strokes would be caused by
supplemental calcium and vitamin D in a group of 100
000 65 year old women, whereas the medium-risk model
predicted about 5000.
Both models showed that the number of years of
high-quality life lost by taking calcium was higher
than the number of years of high-quality life saved
by preventing broken bones.
The study also investigated the cost-effectiveness
of offering 65-year-old women supplemental calcium
and vitamin D assuming that the women were at a low
risk of cardiovascular problems and concluding that
providing supplements in this situation is
cost-effective and good for public health, given
that the benefits outweigh the risks.
However, if the supplement increases risk of heart
attack and stroke, both the savings and the public
health benefit are lost.
“However, if we provide a preventative osteoporosis
medication in addition to a supplement, it will
increase the effect on preventing bone fractures,
and have a positive risk/gain ratio, resulting in
reduced costs,” says Hagen.
The researchers point out that it isn’t possible to
conclude that calcium increases risk of
cardiovascular disease, and that the analysis needs
to be seen in light of this uncertainty.
At the same time, their models are simplifications
that can’t replace studies done on actual people.
“We don’t know for sure if calcium has this negative
effect, but to be careful, we should choose to give
another treatment to help prevent broken bones in
older women,” says Hagen.
For more information
The predicted lifetime costs and health consequences
of calcium and Vitamin D supplementation for
fracture prevention—the impact of cardiovascular
effects. Published in Osteoporosis International, 4
February 2016 (online) Hagen, G., Wisløff, T., &
Kristiansen, I. S. (2016). The predicted lifetime
costs and health consequences of calcium and vitamin
D supplementation for fracture prevention—the impact
of cardiovascular effects. Osteoporosis
International, 1-10.
Link...
MDN |