A new technique can distinguish between
different types of chronic obstructive pulmonary disease (COPD) and
track disease progression. The method could allow for more accurate
diagnoses and lead to more effective treatments for COPD.
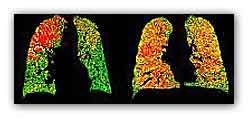
PRM images can help distinguish
healthy lung areas (green) from those with early-stage damage
(yellow) and emphysema (red). Image courtesy of University of
Michigan Center for Molecular Imaging.
PRM images can help distinguish healthy
lung areas (green) from those with early-stage damage (yellow) and
emphysema (red). Image courtesy of University of Michigan Center for
Molecular Imaging.
COPD is a lung disease that makes it
hard to breathe. In people who have COPD, airway tubes to the lungs
narrow, making it hard to get air in and out. COPD can cause
wheezing, shortness of breath, chest tightness and coughing that
produces large amounts of mucus. Cigarette smoking is the leading
cause of COPD in the United States, but the disease can have other
roots as well.
COPD can involve damage to the small
airways of the lungs (functional small airways disease) as well as
destruction of lung tissue (emphysema).
The ability to diagnose the extent of lung damage could help doctors
track disease progression and personalize COPD treatments. Current
CT scan methods can assess the extent of emphysema, but measuring
functional small airways disease has remained a challenge.
Researchers at the University of
Michigan led by Dr. Brian D. Ross set out to address the problem by
adapting an image analysis technique called parametric response
mapping (PRM) that they’d first developed to track tumors.
In PRM, a computer matches voxels—the smallest measureable unit of
volume in an image data set—between CT scans. Voxels in scans taken
during a full inhalation are matched with equivalent voxels in scans
taken during a full exhalation. The density of healthy lung tissue
changes more between the 2 states than the density of diseased lung
tissue. By comparing densities in each voxel pair, a computer
program can create 3-D maps of damage throughout the entire lung.
The scientists analyzed whole-lung CT
scans of 194 people with COPD acquired at both full inhalation and
full exhalation in the COPDGene study, which is funded by NIH's
National Heart, Lung and Blood Institute (NHLBI). Additional funding
was provided by NIH's National Cancer Institute (NCI) and National
Institute of Biomedical Imaging and Bioengineering (NIBIB). Results
appeared online on October 7, 2012, in Nature Medicine.
The researchers showed that PRM could
successfully identify the extent of both functional small airways
disease and emphysema. They also observed a pattern in the data
suggesting that functional small airways disease may precede
emphysema in the progression of COPD.
To investigate whether PRM could be used
to track disease progression, the researchers analyzed images from
people who had undergone inspiratory/expiratory CT scanning over a
period of time. They found that PRM could be used to monitor COPD
progression.
“Essentially, with the PRM technique,
we've been able to tell sub-types of COPD apart, distinguishing
functional small airway disease from emphysema and normal lung
function,” Ross says. “We believe this offers a new path to more
precise diagnosis and treatment planning and a useful tool for
precisely assessing the impact of new medications and other
treatments.”
For more information
Computed tomography-based biomarker provides unique signature for
diagnosis of COPD phenotypes and disease progression
http://www.ncbi.nlm.nih.gov/pubmed?term=23042237 (MDN) | ![]()